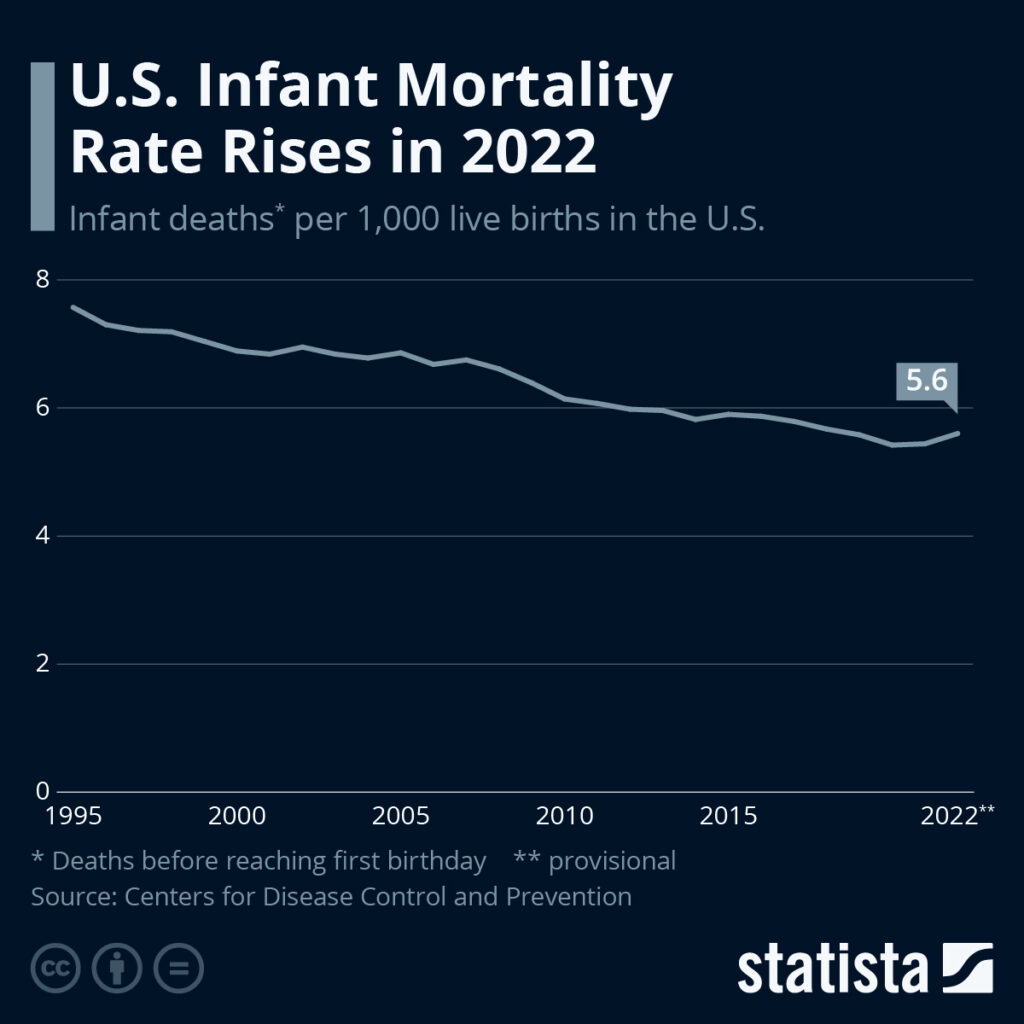
The Centers for Disease Control reports a 3 percent increase in infant mortality in the U.S., reaching 5.6 deaths per 1,000 live births. This uptick represents a trend that had a nearly continuous decline since 1995.
Infant mortality, defined as the death of a child before its first birthday, saw a more significant increase in the 2-11 month age group, with a 4 percent rise, while neonatal deaths (birth to 28 days) increased by 3 percent.
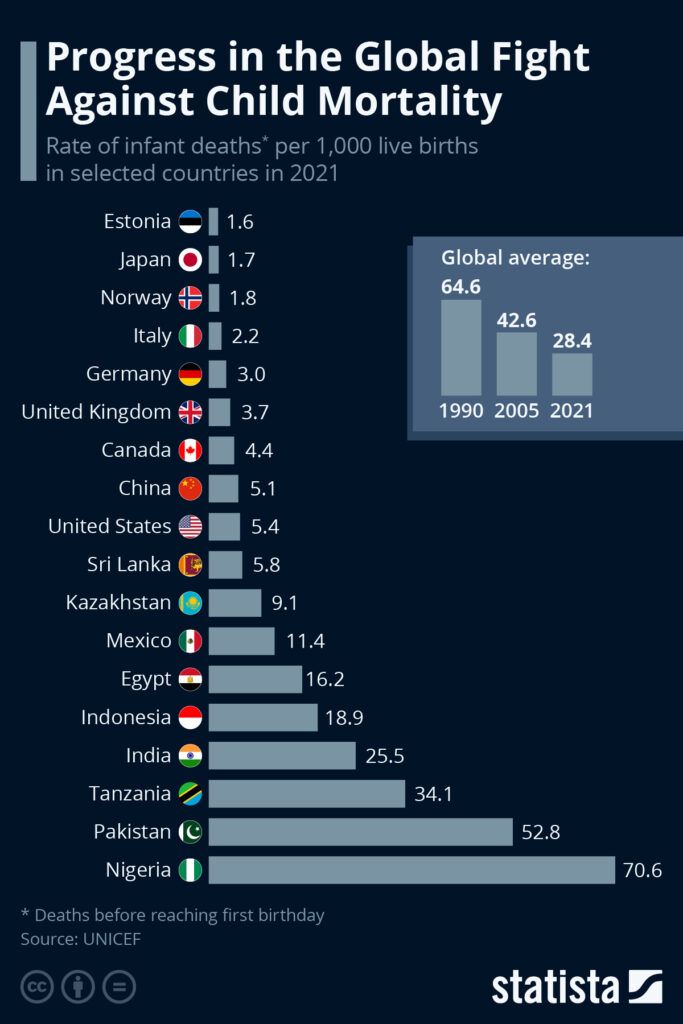
The U.S. lags behind most wealthy countries, including Estonia, Japan, the United Kingdom, and China, while barely beating Sri Lanka in preventing infant deaths.
Lacking Consensus
Experts have not agreed on the reasons for this increase but have proposed several factors. These include a rise in infectious diseases post-social distancing, the continuation of unwanted pregnancies due to abortion restrictions, an increase in maternal complications from COVID-19, and a higher number of women entering pregnancy with pre-existing conditions such as obesity, diabetes, and high blood pressure.
In addition, the reasons for the change in infant mortality in the United States could be multifaceted, involving healthcare system factors, social determinants of health, public health policy, and broader societal changes.
Improve Access
Access to prenatal and pediatric care may also be a factor, as often seen in poorer urban environments and rural areas. Due to the high cost of medical training, graduating medical students gravitate to higher-paying specialties rather than pediatrics, creating a shortage of treating physicians.
Addressing this issue may require a comprehensive approach, including improving access to quality prenatal and postnatal care, addressing health disparities, enhancing infectious disease control, supporting maternal health before and during pregnancy, and establishing incentives for medical graduates to enter primary care specialties.
I look forward to your thoughts, so please submit your comments in this post. And subscribe to my weekly newsletter, “What’s Your Take?” on DocsNetwork.com.